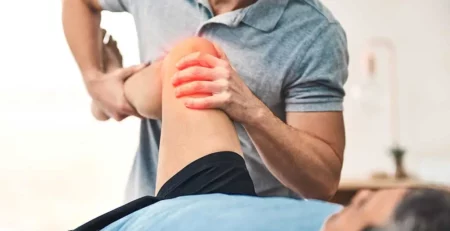
You’re not the only one who has experienced unexpected bladder leaks, chronic lower back pain, or discomfort during intimate moments. Affecting 1 in 4 women, Pelvic Floor Dysfunction is still one of the problems that receives the least amount of attention. The good news? Most people show noticeable improvement in a matter of weeks with the correct strategy.
The first step to healing is realizing what’s going on in your body. Let’s examine how to recognize the symptoms of pelvic floor dysfunction, do a home test, and follow a treatment plan.
What Is Pelvic Floor Dysfunction?
The muscles that reach from the pubic bone to the tailbone make up the pelvic floor, which resembles a hammock. These muscles control urination, bowel motions, and sexual function in addition to supporting your bladder, uterus.
This occurs when muscles become weak, tight, or lose coordination. It’s interesting to note that weakness isn’t always the issue; sometimes it’s the other way around.
Understanding Your Pelvic Floor Muscles
Your pelvic floor is a group of muscles and ligaments that form a supportive sling at the base of your pelvis. These muscles control bladder and bowel activity and help stabilize your hips and core.
How the Pelvic Floor Works
When working properly, pelvic muscles tighten to prevent leakage and relax to allow proper emptying. Dysfunction occurs when these muscles become weak (hypotonic) or overly tight (hypertonic).
Who Is Most at Risk
- Postpartum women (especially after difficult deliveries)
- People recovering from pelvic or abdominal surgery
- Those with chronic constipation or straining
- Athletes performing high-impact workouts
- Older adults due to natural muscle weakening
Two main types exist:
- Hypotonic (weak) pelvic floor – muscles are stretched or weakened
- Hypertonic pelvic floor – muscles are overly tight and can’t relax properly
People actually have a hypertonic pelvic floor, where their symptoms are caused by tension rather than weakness, according to the Cleveland Clinic. This is why traditional Kegel exercises sometimes make things worse.
Common Pelvic Floor Dysfunction Symptoms
Early recognition of the symptoms improves the effectiveness of treatment. Furthermore, symptoms may appear gradually, which makes it simple to write them as “natural aging” or “just part of being a woman.”
Bladder and bowel symptoms:
- Urinary urgency or frequency (rushing to the bathroom constantly)
- Stress incontinence (leaking when you cough, sneeze, or exercise)
- Difficulty starting urination or incomplete emptying
- Constipation or straining during bowel movements
- Accidental bowel leakage
Pain and discomfort:
- Chronic lower back pain, hip, or pelvic pain
- Painful intercourse (dyspareunia)
- Tailbone pain that worsens when sitting
- Unexplained pressure or heaviness in the pelvis
Pelvic organ prolapse symptoms:
- A bulge or fullness in the vaginal area
- Sensation that something is “falling out”
- Worsening symptoms after standing for long periods
According to the NHS, early detection is essential since pelvic floor dysfunction problems frequently get worse without treatment. However, people significantly improve with appropriate pelvic health care.
What causes pelvic floor dysfunction?
Experts don’t know the exact cause of pelvic floor dysfunction, but several factors may contribute to it:
- Pelvic injuries from accidents or falls.
- Overuse of pelvic muscles, such as frequent straining during bowel movements.
- Previous pelvic surgeries (e.g., hysterectomy or prostatectomy).
- Pregnancy and childbirth, especially in difficult deliveries.
- Aging which weakens muscles over time.
- Stress and anxiety can increase muscle tension.
- Connective tissue disorders affect the strength of muscles and ligaments.
Pelvic Floor Self-Test: Assess Your Symptoms at Home
You can assess your muscle function by doing a quick pelvic floor dysfunction self-test before making an appointment. Although it doesn’t take the place of professional evaluation, this offers insightful information.
Pelvic Muscle Awareness Test
While lying down, try gently tightening the muscles used to stop urine flow — without moving your legs or abdomen. Difficulty controlling them may indicate dysfunction.
Balloon or Straining Test
If you often feel the need to push hard to pass stool or gas, your pelvic muscles may not be relaxing properly.
Breathing and Relaxation Awareness
Notice if you “hold tension” in your belly or breath. Shallow or chest breathing can worsen pelvic tightness.
Strength and coordination test:
- Wash your hands thoroughly
- Lie down in a comfortable, private space
- Insert one clean finger into your vagina (about 2 inches)
- Squeeze your pelvic floor muscles as if stopping urine midstream
- Notice the strength, duration, and quality of the contraction
What to look for:
- Weak response – Little to no squeeze sensation suggests hypotonic muscles
- Can’t relax – If muscles feel constantly tense, you may have a hypertonic pelvic floor
- Uneven contraction – One side feels stronger than the other
- Quick fatigue – Can only hold for 1-2 seconds before muscles give out
Functional tests to try:
- Jump test – Jump 10 times; any leaking suggests stress incontinence
- Cough test – Cough forcefully with a full bladder
- Endurance test – Try holding a pelvic floor contraction for 10 seconds
It is essential to see a pelvic floor physical therapy professional if you feel pain during a pelvic floor dysfunction self-test. They are able to offer accurate evaluations and personalized treatments.
Conditions Commonly Confused with Pelvic Floor Dysfunction
Because pelvic floor symptoms often mimic other conditions, many people are misdiagnosed or treated for the wrong issue. The following are some of the most common conditions mistaken for pelvic floor dysfunction:
- Irritable Bowel Syndrome (IBS) – Causes abdominal pain and irregular bowel movements.
- Interstitial Cystitis (IC) – Bladder pain and urgency without infection.
- Pelvic Organ Prolapse (POP) – Pelvic organs descend due to weak support.
- Chronic Constipation / Fissures – Often overlap with muscle tension issues.
Understanding Your Pelvic Floor Type
Depending on how tight or loose your muscles are, the course of treatment can differ widely. Unfortunately, people believe they need to “strengthen” when, in reality, they need to relax.
Signs of a hypertonic (tight) pelvic floor:
- Pain during intercourse or pelvic exams
- Difficulty starting urination despite urgency
- Chronic constipation
- Tailbone or hip pain
- Paradoxical incontinence (leaking despite “strong” muscles)
Therefore, typical Kegel exercises may worsen symptoms and increase tension if you have a hypertonic pelvic floor. Instead, you need to stretch gently and use relaxation techniques.
Signs of a hypotonic (weak) pelvic floor:
- Leaking with physical activity
- No sensation during the self-test
- Pelvic organ prolapse
- Feeling like you can’t “find” or activate the muscles
Progressive strengthening exercises serve as your foundation in this situation. However, for healthy function, even the strongest pelvic floor dysfunction exercises need to include relaxation.
The 12-Week Pelvic Floor Rehab Plan
Both weakness and tension are addressed by this evidence-based therapy. The American College of Obstetricians and Gynecologists (ACOG) recommends that planned rehabilitation is more effective than random activities.
Weeks 1-4: Foundation & Awareness
Primary focus: Learning proper muscle engagement and breathing
Daily routine (10-15 minutes):
- Diaphragmatic breathing – 5 minutes lying down, hand on belly
- Pelvic floor awareness – 10 gentle contractions, holding 3 seconds each
- Release practice – Consciously relax muscles between contractions
- Posture check – Sit and stand with neutral spine alignment
Key exercises:
- Happy Baby Pose – Lie on back, knees to chest, hold ankles (hold 2 minutes)
- Child’s Pose – Kneel and stretch forward, focus on pelvic floor release (2 minutes)
- Cat-Cow Stretch – Coordinate breathing with spinal movement (10 rounds)
Additionally, start keeping a journal to record your symptoms. Take note of the frequency of leaks, the level of pain, and any patterns you notice.
Weeks 5-8: Building Strength & Coordination
Primary focus: Progressive muscle training with proper form
Daily routine (15-20 minutes):
- Quick flicks – 20 rapid contractions (1 second each)
- Endurance holds – 10 contractions held for 6-8 seconds
- Functional integration – Practice engaging muscles before sneezing/coughing
- Hip strengthening – Clamshells and bridges (2 sets of 15 reps)
Biofeedback therapy consideration:
According to research, biofeedback therapy greatly enhances results. These help you develop proper engagement by giving you audio or visual feedback about your muscles. Additionally, research shows that combining biofeedback with physical therapy has an 80% success rate.
Key exercises:
- Bridge with Hold – Lift hips, squeeze pelvic floor, hold 10 seconds (10 reps)
- Wall Squats – Contract pelvic floor at the bottom of the squat (12 reps)
- Standing Marches – Maintain engagement while lifting knees (20 total)
Weeks 9-12: Functional Training & Real-World Application
Primary focus: Returning to activities without symptoms
Daily routine (20-25 minutes):
- Dynamic movements – Lunges, step-ups with pelvic floor engagement
- Impact progression – Low jumping activities if appropriate
- Core integration – Planks and modified abdominal exercises
- Stretching routine – Maintain flexibility gains (10 minutes)
Progressive challenges:
- Return to exercise gradually (walking → jogging → running)
- Practice sneezing/coughing with engagement
- Increase functional activities (lifting children, groceries)
- Test symptom improvement with previous trigger activities
Meanwhile, keep avoiding activities that worsen symptoms. Pay attention to your body; if it’s uncomfortable, you’re pushing too hard.
When to Seek Pelvic Floor Dysfunction Physical Therapy
While people benefit from at-home exercises, expert pelvic floor physical therapy speeds up healing. Consider scheduling an evaluation if:
- Symptoms persist after 4-6 weeks of consistent home exercise
- You experience pain during exercises
- You’re unsure whether you have a hypertonic or hypotonic pelvic floor
- You’re preparing for or recovering from postpartum recovery
- You have pelvic organ prolapse
To develop personalized treatment plans, specialized therapists use biofeedback therapy, ultrasound imaging, and internal assessment methods. Due to research, trained pelvic floor physical therapy actually reduces symptoms twice as quickly as at-home programs.

Lifestyle Modifications That Support Healing
Beyond exercises, several daily habits impact your recovery:
Dietary considerations:
- Stay hydrated (but don’t overdo it)
- Reduce bladder irritants (caffeine, alcohol, acidic foods)
- Increase fiber to prevent constipation
- Avoid straining during bowel movements
Movement patterns:
- Practice proper lifting mechanics (engage core first)
- Avoid high-impact exercise until symptoms improve
- Take regular movement breaks if you sit all day
- Maintain a healthy weight to reduce pelvic pressure
Stress management:
Pelvic floor tension grows due to chronic stress. As a result, using relaxation methods like yoga, meditation, or gentle stretching helps healing and muscle release.
Evidence-Based Treatments and Therapies
Pelvic Floor Physical Therapy (PFPT)
The gold-standard approach. Therapists use manual techniques, guided exercises, and relaxation methods to restore balance.
Biofeedback and Electrical Stimulation
Real-time muscle feedback helps retrain coordination. Gentle stimulation may help weak muscles contract properly.
Relaxation and Stress-Relief Techniques
Yoga, breathing, and mindfulness help reduce tension and support long-term muscle recovery.
Trigger Point Injections and Pain Management
Used for severe spasms or chronic pain unresponsive to therapy.
Lifestyle and Posture Corrections
Improving sitting posture, toilet habits, and lifting techniques can greatly reduce symptoms.
Medical or Surgical Options
Surgery is rare and only for structural issues like prolapse or nerve entrapment.
What Research Says
Studies show over 75% improvement with consistent PFPT and biofeedback therapy within 3–6 months.
Your Path to Recovery Starts Now
The symptoms of pelvic floor dysfunction don’t have to rule your life. People who use pelvic floor dysfunction exercises consistently notice improvement after 4-6 weeks. The 12-week pelvic floor rehab course offers an organized approach to healing.
Remember that healing isn’t always simple. It’s common for some days to feel better than others. Remain patient with your body, celebrate little achievements, and don’t be afraid to seek pelvic floor physical therapy if you require further assistance.
Your pelvic floor has supported you at the most difficult moments in your life. Take the pelvic floor dysfunction self-test now, start your rehabilitation exercises tomorrow, and observe how your symptoms slowly go away.
Take that first step, your future self will thank you.
Why Choose Pelvic Floor Rehab at Body & Mind Osteopathic Clinic?
At Body & Mind Osteopathic Clinic, we take a holistic and evidence-based approach to treating pelvic floor dysfunction—combining osteopathy, physiotherapy, and guided home programs for lasting recovery.
-
Certified pelvic floor therapists with advanced training in both men’s and women’s pelvic health
-
Personalized 12-week rehab plans designed for your specific symptoms and goals
-
Integrated treatment approach using physical therapy, biofeedback, and relaxation techniques
-
Convenient Toronto and Vaughan locations, ideal for anyone searching “pelvic floor therapy near me”

Written By: Vadzim Siniauski
Vadzim Siniauski is Certified Osteopathic manual practitioner DOMP, MCIO, and Registered Massage Therapist (RMT), MD (Belarus). Vadzim has an extensive experience in musculoskeletal health, pain management, and manual therapy techniques.
Our Editorial Process
At Body & Mind Osteopathic Clinic, we publish practical, experience-based content to help educate readers on osteopathy, rehabilitation, and wellness.
Writing: All our content is developed by experienced osteopathic practitioners and RMTs. It draws on reputable scientific literature, clinical research, and our real-world experience working with conditions such as back pain, joint stiffness, postural imbalances, and injury recovery.
Editing: Each article is reviewed internally by a senior practitioner to ensure accuracy, clarity, and alignment with our treatment protocols and patient education standards.
Verified by Practitioners: Before publication, content is verified by a licensed member of our clinical team to confirm that the medical information provided aligns with current best practices in manual therapy and osteopathic care.
Frequently Asked Questions
What Is the Main Cause of Pelvic Floor Dysfunction?
Often from muscle imbalance, overstraining, or surgery-related weakness.
How can I tell if I have pelvic floor dysfunction?
You can tell if you have pelvic floor dysfunction by taking a self-test that assesses symptoms such as difficulty emptying the bladder, pelvic pressure, pain during intercourse, and bowel movement issues. Scoring above a certain threshold indicates likely dysfunction and the need for professional evaluation.
Is there a self-test for pelvic floor dysfunction?
Yes, there is a 10-question pelvic floor dysfunction self-test that helps identify symptoms based on severity and frequency. A score of 5 or more suggests significant dysfunction, indicating the need for further assessment and a rehab plan.
Are There Home Biofeedback Devices?
Yes — several safe, app-based tools track contraction strength and relaxation.
Can pelvic floor dysfunction be treated without surgery?
Yes, pelvic floor dysfunction can be treated without surgery using conservative methods like physiotherapy, breathing retraining, and daily movement plans. Most patients improve significantly with these techniques, avoiding the need for surgical intervention.
When Should I See a Specialist?
If symptoms persist beyond 6–8 weeks or cause pain, seek a pelvic health specialist.